Aetna Health North Star
The North Star is a user-centered experience framework for Aetna Health - focused on modular “journeys” that guide the member in their moments of care. Utilizing our core business strategy and key insights, we can redefine how people use their benefits and become their health insurance guide- their health champion.
Healthcare benefits pain points persist because we haven’t yet imagined a truly valuable digital tool to successfully navigate the complex healthcare and insurance system.

THE PROBLEM
USER EXPERIENCE
- Disconnected experiences based on outdated mental models lead to siloed tools
- Little guidance in confident decision making
- No sense of value or incentive to engage
- Old data architecture and tech stacks don’t align with how people experience health journeys
- Too many data sources in healthcare cause deep fragmentation in tools and experiences
- No automation or intelligence to handle complex tasks
BUSINESS NEEDS
- Business outcomes are dependent on member engagement, education, and confidence in decision making, keeping members healthier and costs down
- Aetna needs market differentiation from other basic health insurance experiences to retain and expand membership in key areas
- Increase CVS Digital customer footprint, Improve customer experience for relevant ETMMs, contribute to an overall call reduction across all business units
STRATEGY & SOLUTION
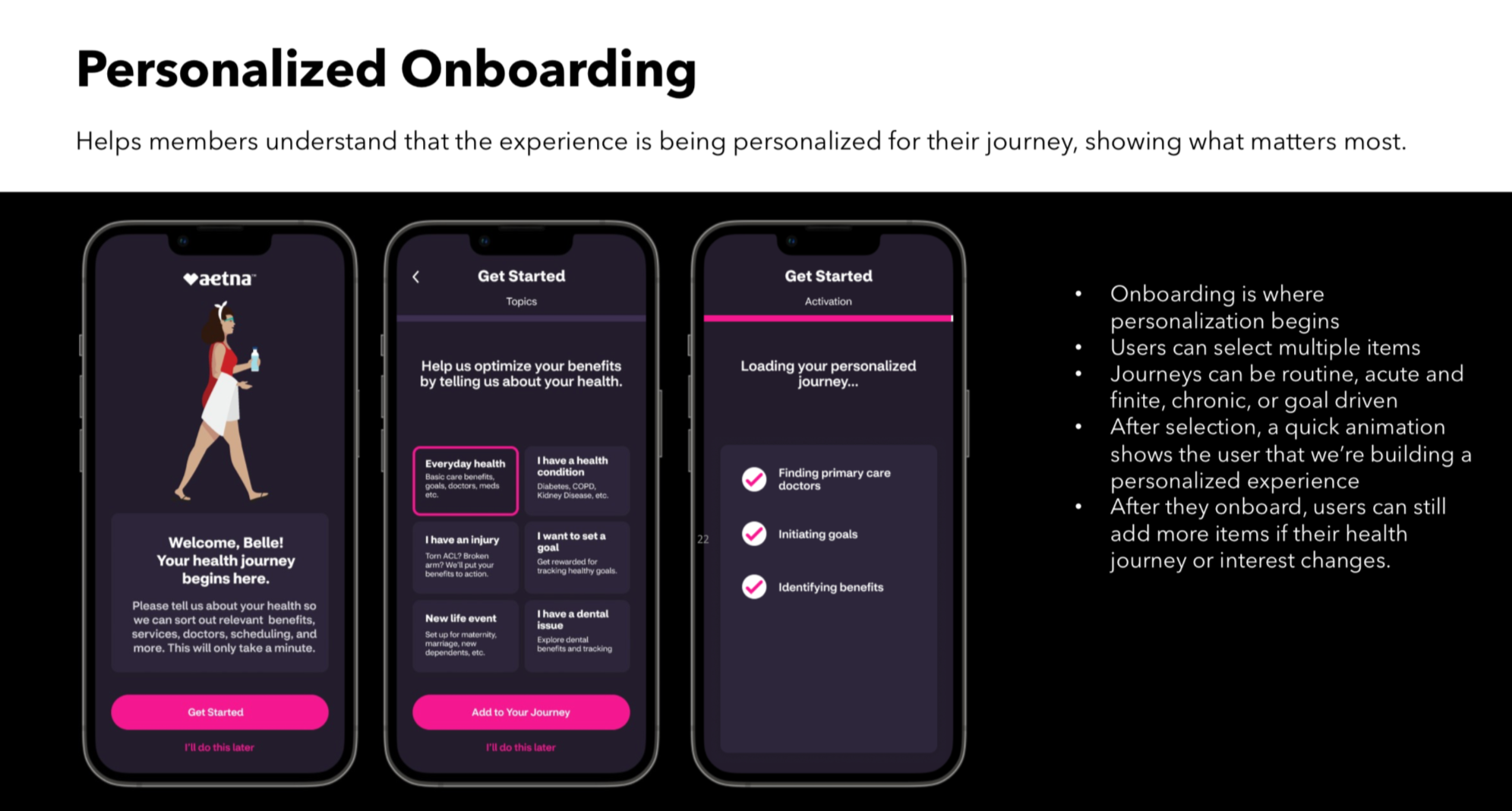
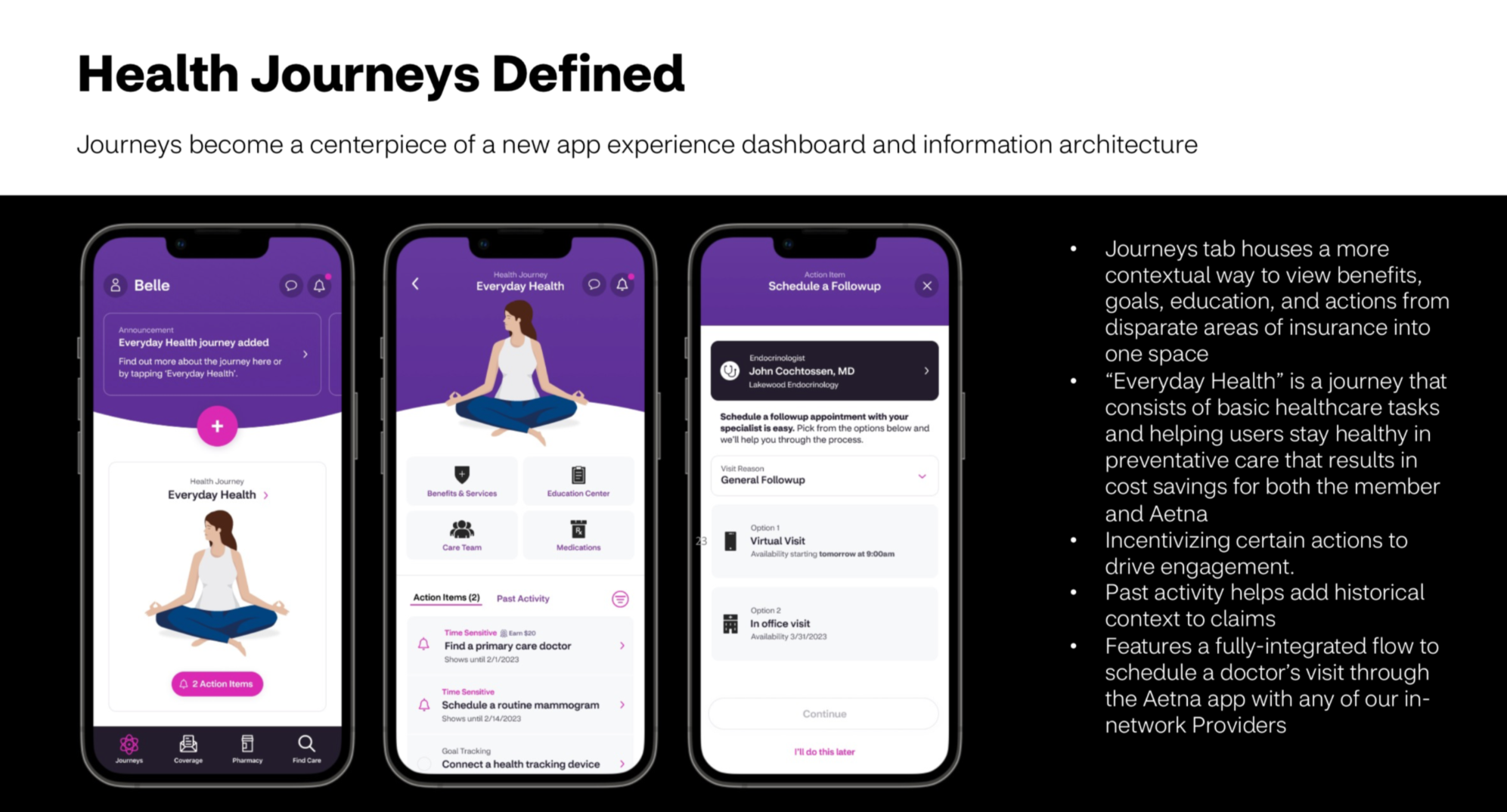
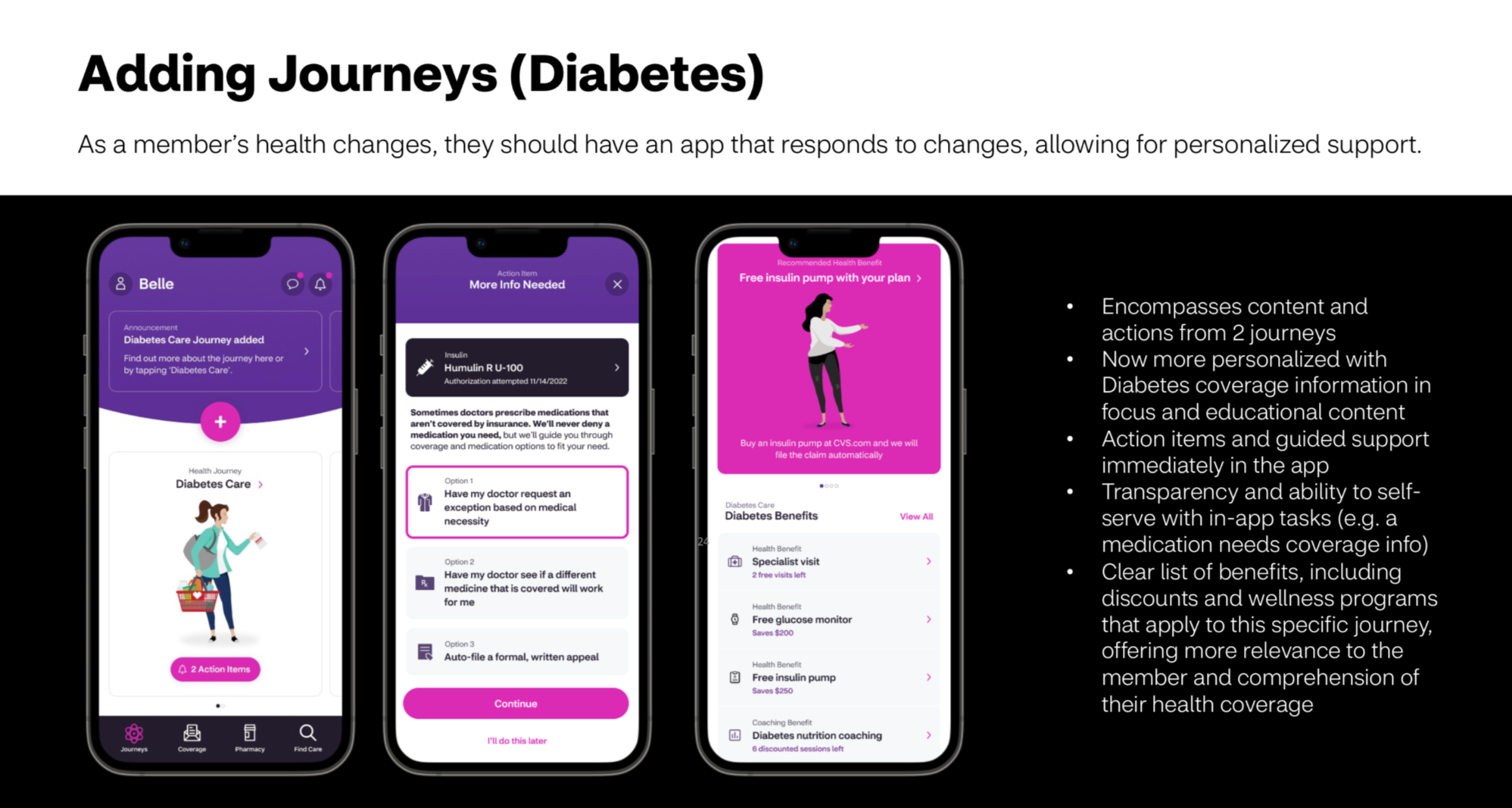
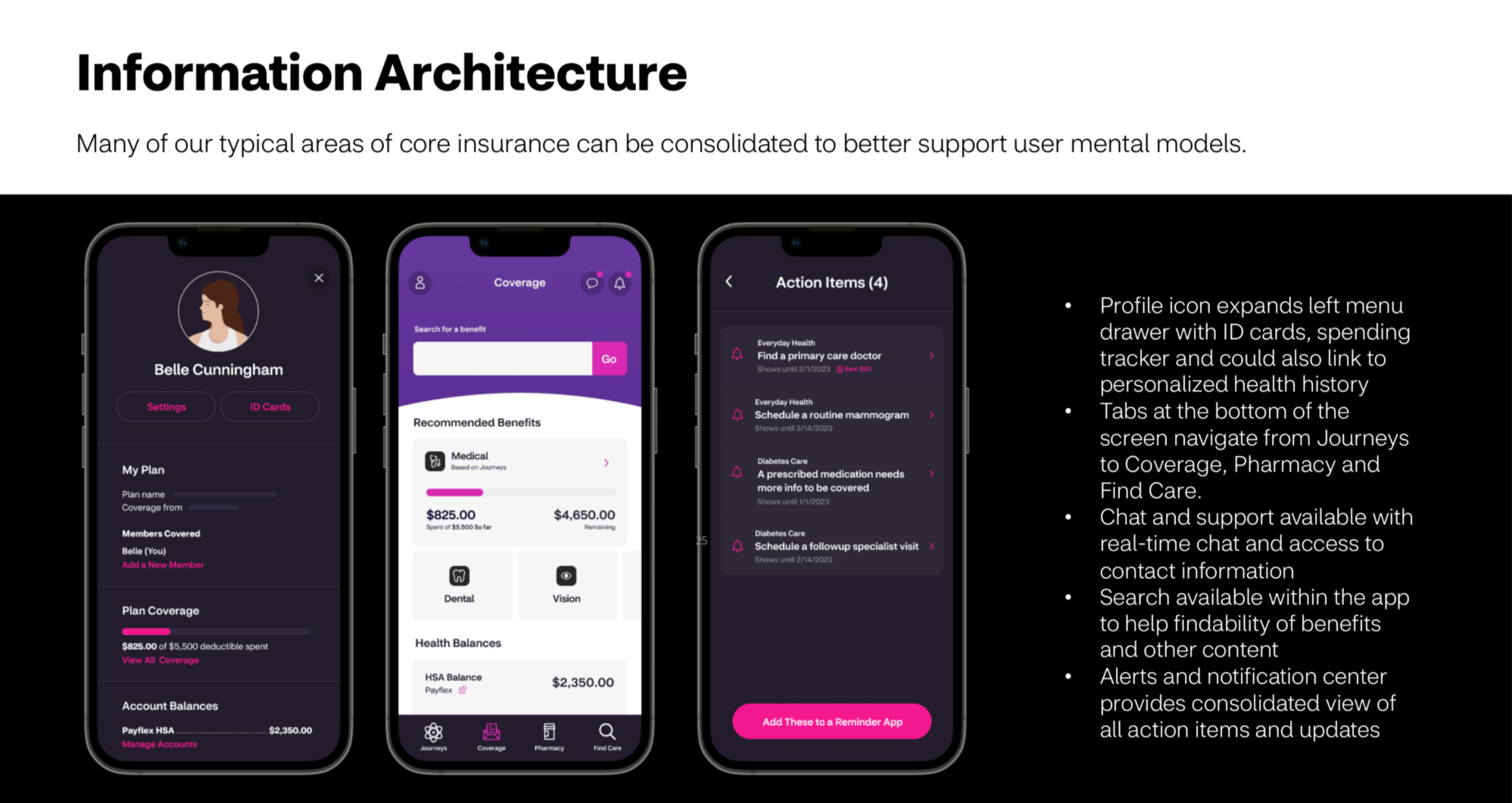
If we group contextual benefit information, healthy actions, and program education into guided experiences, while incentivizing members to use these guides, they will be able to self service more confidently, make more informed health and benefit decisions, and more actively engage with the online experience. This will lead to healthier outcomes for them and better business outcomes for Aetna and its partners.
EXPERIENCE THE PROTOTYPE